The hardest stage of menopause isn’t what most women expect. Many assume the worst comes after their periods stop, but in reality, the most intense and overwhelming phase often happens before that point. Understanding what the hardest stage of menopause is can make the difference between feeling lost and feeling prepared.
If you’re starting this journey. It’s important to understand the difference between perimenopause and menopause. Perimenopause vs Menopause
Here’s something nobody tells you: the finish line isn’t where you think it is. Most women brace themselves for menopause itself, expecting relief afterward. But the real challenge builds quietly before that moment arrives.
Why late perimenopause is the hardest stage of menopause
If you’ve been wondering what the hardest stage of menopause is, the answer may surprise you: late perimenopause,
This phase usually occurs 1 to 3 years before your final period, and it’s widely considered the hardest stage of menopause because of extreme hormonal instability.
Why does this phase hit so hard? During late perimenopause, your estrogen levels don’t just decline gradually; they swing dramatically from day to day, sometimes hour to hour. One moment, you might have nearly normal estrogen levels, and the next, they’ve plummeted. Your body struggles to adapt to this unpredictability, and that’s what creates those intense symptoms everyone talks about.
What makes late perimenopause particularly brutal is how multiple symptoms pile on simultaneously. Poor sleep due to night sweats exacerbates mood changes, and hormonal chaos affects concentration. The sheer unpredictability leaves you feeling like you’re losing control of your own body. But here’s what I want you to know: you have more power than you think to ease this transition through simple, everyday lifestyle choices.
What makes the hardest stage of menopause so Intense
During the hardest stage of menopause, symptoms don’t just appear—they pile up all at once.
- Severe hot flashes and night sweats
- Chronic fatigue and low energy
- Mood swings and anxiety
- Brain fog and poor concentration
- Sleep disruption
Research shows that up to 80% of women experience severe hot flashes and night sweats during this phase. Many women dealing with menopause fatigue describe this period as the most exhausting of the entire transition.
What makes the hardest stage of menopause particularly brutal is the combination of symptoms. Poor sleep leads to fatigue, which worsens mood swings, increases stress, and pauses the cycle
The good news? Even during the hardest stage of menopause. Small lifestyle changes can make a difference.
Start Your Morning Right
Your breakfast matters more than ever now. A plate that stabilizes blood sugar and supports hormone balance. Greek yogurt (plain, not sweetened) topped with a handful of walnuts and fresh berries, or try two scrambled eggs with avocado on whole-grain toast, a side of sautéed spinach. The Mediterranean diet breakfast approach works beautifully here.
Healthy fats, protein, and fiber keep your energy steady.
Add these vital vitamins women 50 need at breakfast through real food first. That yogurt? Is it giving you calcium and vitamin D? Those walnuts? Omega-3s for brain health and mood stability, spinach, and Magnesium help with sleep and reduce anxiety.
Move Your Body Gently
You don’t need intense workouts. A 30-minute daily walk or light strength training twice a week can improve mood, metabolism, and energy levels.
Strength training is especially powerful at this stage. Here’s how to start Strength Training safely After 50 for Women.
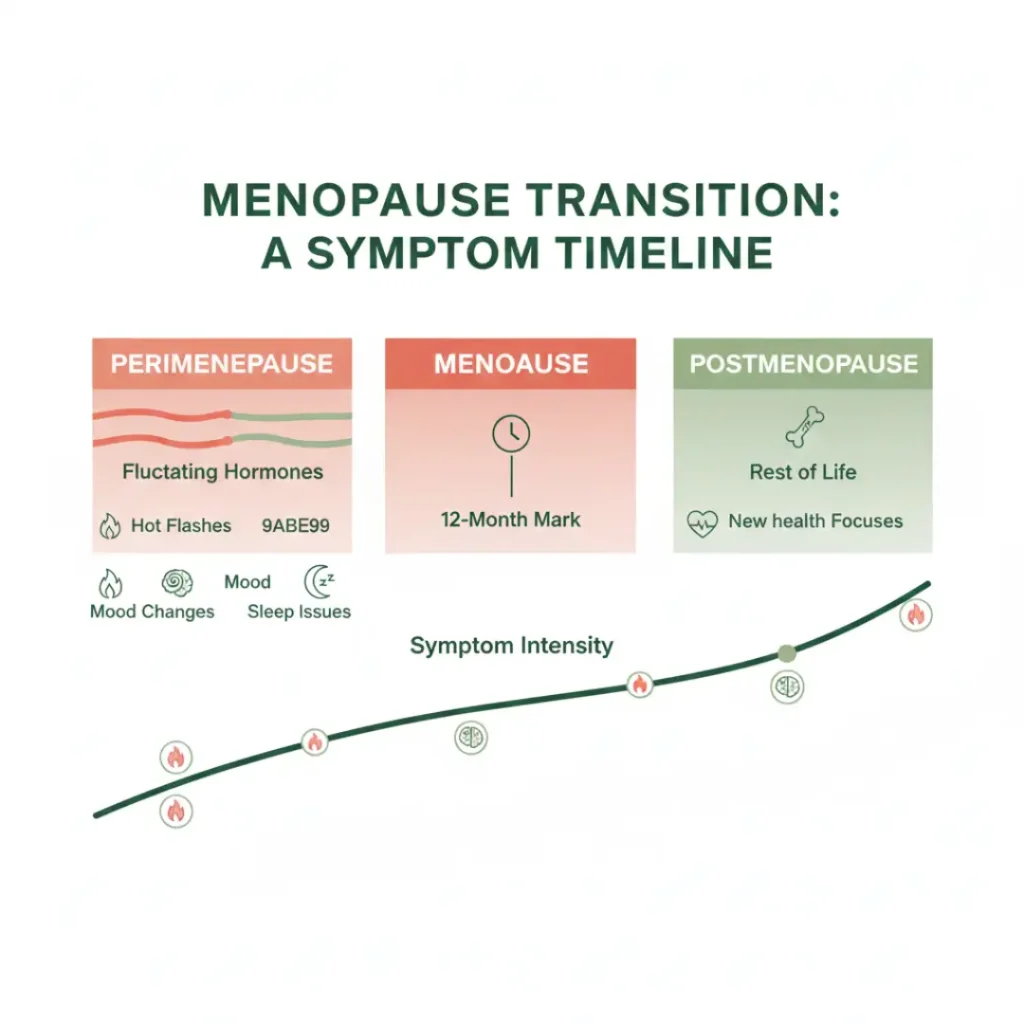
Managing hot flashes during the hardest stage of menopause
Hot flashes are one of the most frustrating parts of the hardest stage of menopause, but they can be managed.
Let’s discuss hot flashes during menopause and the lifestyle strategies that truly help. Medical treatments, but these practical adjustments can reduce frequency and intensity.
Your wardrobe becomes a tool. I keep three layers ready every morning: a breathable cotton camisole, a button-front cardigan ( to remove quickly), and a lightweight scarf or jacket. Natural fabrics, cotton, linen, and bamboo, allow your skin to breathe. Avoid polyester and other synthetics that trap heat and moisture.
Keep a “hot flash kit” in your bag: a small battery-powered fan, cooling wipes, and a water bottle. I learned this from a friend who swore it saved her during business meetings. When a flash hits, having these tools within reach makes it manageable instead of mortifying.
Temperature control at home and work. Set your bedroom thermostat between 60-67°F at night. Yes, it’s cold, but it’s optimal for sleep during this phase. Invest in moisture-wicking sheets (bamboo or special athletic fabric) and keep a cooling pillow on hand. Layer blankets so you can adjust easily when night sweats hit.
At work, position yourself near windows you open or away from heat sources. Keep a small desk fan handy. If you work from home, this is easier to control; embrace it.
Trigger awareness changes everything. Start tracking what sets off your hot flashes. Common culprits include spicy foods, hot beverages, alcohol (especially red wine), caffeine after 2 PM, and stress. You don’t have to eliminate everything forever, but knowing your triggers helps you make conscious choices. Maybe you skip the spicy curry on days when you have important meetings scheduled.
Sleep strategies that actually work
Understanding why sleep problems increase after age 50 helps you tackle them; hormonal fluctuations directly impact sleep architecture, but your evening routine can work with your body instead of against it.
Create a cooling bedtime ritual. About an hour before bed, take a lukewarm shower, not hot, which slightly lowers your core body temperature, signaling time. Follow with a lightweight, breathable nightgown or pajamas, and keep a second set on your nightstand for when night sweats require a change.
Your bedroom should become a sleep sanctuary. Remove electronic devices; the blue light disrupts melatonin production, which is already compromised by hormonal changes. Use blackout curtains or an eye mask. Consider a white noise machine to mask disruptive sounds that wake you during lighter sleep phases.
The 3-2-1 rule works wonders: No food 3 hours before bed (prevents acid reflux that worsens with hormonal changes), no liquids 2 hours before bed (reduces nighttime bathroom trips), no screens 1 hour before bed (protects melatonin production). Replace evening scrolling with reading, gentle stretching, or journaling.
If night sweats wake you, don’t just lie there frustrated. Get up, change your clothes if needed, do some gentle stretches, sip cool water, and return to bed. Fighting wakefulness creates anxiety around sleep, making the problem worse.
Nutrition and supplements: your daily defense
What you eat directly impacts how you feel during the hardest stage of menopause. Let me be specific about what helps.
Build every meal around these principles: Protein (aim for 25-30 grams per meal to maintain muscle mass and stabilize blood sugar), healthy fats (avocado, olive oil, nuts, fatty fish), and fill half your plate with vegetables. This combination keeps you satisfied longer and reduces those energy crashes that make everything feel harder.
Certain foods deserve special mention. Flaxseeds contain lignans that may help with hot flashes. Grind them fresh and add a tablespoon to your morning smoothie or yogurt. Soy foods (edamame, tofu, tempeh) contain phytoestrogens that some women find. Cold-water fatty fish (salmon, sardines, mackerel) provide omega-3s that support mood and reduce inflammation.
What to minimize: Refined sugars and simple carbs cause blood sugar spikes and crashes that worsen mood swings and energy fluctuations. Alcohol, especially in the evening, disrupts sleep quality even if it helps you fall asleep initially. Excessive caffeine intensifies anxiety and triggers hot flashes in many women.
Consider these supplements for perimenopause and beyond after discussing with your doctor: Vitamin D3 (2000-4000 IU daily) with K2 for bone health, magnesium glycinate (300-400mg before bed) for sleep and muscle relaxation, omega-3 fatty acids (1000-2000mg daily) for mood and heart health, and a quality B-complex for energy support.
Stress management: your secret weapon
Stress amplifies every menopause symptom. When you’re stressed, cortisol levels spike. The good news? Simple stress management practices make a measurable difference.
Practice 4-7-8 breathing when hot flashes strike: Breathe in through your nose for 4 counts, hold for 7 counts, exhale through your mouth for 8 counts. This activates your parasympathetic nervous system, helping regulate body temperature and reducing anxiety. Do this three times whenever you feel a hot flash coming or when stress peaks.
Gentle yoga, especially restorative poses. You don’t need an hour-long class. Even 10 minutes of cat-cow stretches, child’s pose, and legs-up-the-wall pose before bed calms your nervous system. There are wonderful free videos online specifically for menopause symptoms.
Social connection matters more than you think. Isolation makes symptoms feel worse. Schedule regular coffee dates, join a walking group, or online communities of women going through the same thing. Your experience with others who understand reduces the psychological burden significantly.
Set boundaries without guilt. If evening social events exhaust you during this phase, it’s okay to decline. If you need to leave work on time instead of staying late, do it. Protecting your energy isn’t selfish; it’s essential self-care during a demanding transition.
When lifestyle adjustments need medical support
Everything I’ve shared helps, but I want to be clear: lifestyle changes don’t always solve everything, and that’s completely normal. If your symptoms persist despite these adjustments, medical treatment isn’t a failure; it’s smart healthcare.
Hormone replacement therapy can be life-changing for women struggling with severe symptoms during late perimenopause. Non-hormonal options exist, too. Some women benefit from antidepressants that reduce hot flash frequency. Others find relief with blood pressure medications that weren’t designed for menopause but happen to help with temperature regulation.
Don’t suffer in silence because you think you “should” be able to manage this naturally. Late perimenopause is intense for biological reasons beyond your control. Combining lifestyle strategies with appropriate medical treatment during this transition.
Talk with a healthcare provider who listens and takes your concerns seriously. If your doctor dismisses your symptoms as “just menopause” without offering solutions, find a new doctor. You deserve support, not dismissal.

Looking toward postmenopause: life gets better
Here’s the hopeful truth about what is the hardest stage of menopause: it’s temporary. Once you cross into postmenopause, that 12-month mark without a period, most women experience significant relief as hormones stabilize at new, lower levels.
Hot flashes typically decrease in frequency and intensity within 2-5 years after your final period. Sleep improves. Energy returns. That brain fog lifts. Many women describe feeling more like themselves again, often with deeper confidence than before.
The lifestyle habits you develop during late perimenopause serve you beautifully in postmenopause and beyond. That morning walk becomes a cherished routine; the Mediterranean-style supports heart and brain health. management practices enhance overall well-being for years to come.
Understanding perimenopause vs menopause and postmenopause helps you recognize that you’re moving toward a phase many women describe as liberating. No more periods. No pregnancy concerns. Often, renewed clarity about what truly matters in life.
If you’re looking for more ways to thrive with energy, confidence, and vitality at 50, remember that this transition, though challenging, can become a gateway to one of your most vibrant decades.
Your next steps
So what is the hardest stage of menopause? For most women, it’s late perimenopause, those intense 1-3 years before periods stop. But you now have specific, practical strategies to ease the journey.
Start with one or two changes rather than trying to overhaul everything overnight. This week, you can focus on your morning routine and sleep environment. Next week, you will adjust your breakfast and add a daily walk. Small, consistent changes compound into significant relief over time.
Track what helps. Keep a simple journal of symptoms, lifestyle adjustments, and how you feel. This helps you identify patterns and gives you concrete information to share with your healthcare provider.
Remember, you’re not alone in this journey. Millions of women navigate this transition every year. The support and information available today far surpass what previous generations had access to. Use it. Reach out. Connect with others. Advocate for yourself.
Always consult with a qualified healthcare provider about your specific symptoms and treatment options. Your experience is unique, and personalized medical advice ensures you get the support that’s right for your body and circumstances.
The hardest stage passes, and what comes next holds genuine possibility for vitality, purpose, and joy. What small lifestyle change will you try first this week?
Frequently asked questions
How long does the hardest stage of menopause last?
Late perimenopause typically lasts 1-3 years before your final period. The entire symptomatic period can extend 4-5 years total when including early postmenopause. Every woman’s timeline differs, so your experience may be shorter or longer. Lifestyle adjustments can help you manage symptoms more comfortably during this window.
Can perimenopause symptoms get worse before they get better?
Yes, absolutely. Many women notice symptoms intensifying as they progress from early to late perimenopause. This worsening actually signals you’re moving through the transition. Once you reach postmenopause, symptoms typically begin to ease. This is why having solid lifestyle strategies in place becomes so important during the peak intensity phase.
What’s the best diet during late perimenopause?
A Mediterranean-style approach is best for most women: of vegetables, fruits, whole grains, healthy fats (olive oil, nuts, avocado), lean proteins, and fatty fish. Focus on blood sugar stability by including protein with every meal, minimizing processed foods and added sugars, and staying well-hydrated. Some women find that reducing caffeine and alcohol helps decrease frequency.
Do I need supplements during the hardest stage of menopause?
Many women benefit from targeted supplements during late perimenopause, including vitamin D3 with K2 for bone health, magnesium for sleep and muscle relaxation, omega-3 fatty acids for mood, and B-complex vitamins for energy; however, supplements should complement a healthy diet, not replace it. Always discuss supplements with your healthcare provider to ensure they’re appropriate for your situation and don’t interact with medications.
Should I see a doctor during late perimenopause?
Absolutely. Even though perimenopause is natural, you don’t have to struggle through severe symptoms alone. A healthcare provider can offer treatments, rule out other concerns, and help you manage symptoms effectively through both lifestyle recommendations and medical options when needed. If symptoms disrupt your daily life, sleep, work performance, or emotional well-being, it’s definitely time to seek professional support.



