I stood in the Target parking lot for fifteen minutes last Tuesday, genuinely unable to remember where I’d parked my car. I walked up and down rows, clicking my key fob, feeling increasingly panicked. When I finally found it, exactly where I always park, I sat behind the wheel and cried. Not because I’d lost my car, but because I was terrified I was losing my mind.
If you’ve experienced something similar, if you’ve walked into rooms and forgotten why, if you’ve blanked on the name of someone you’ve known for years, if you’ve felt like your brain is wrapped in cotton wool, I need you to know something important: you’re not losing your mind. This is perimenopause brain fog, and up to 60 percent of women experience cognitive difficulties during this transition.
What perimenopause brain fog actually feels like
Let me paint you a picture of what this experience looks like in real life, because “brain fog” sounds vague until you’re living it.
You’re in the middle of a presentation at work, and suddenly you can’t find the word you need. It’s right there, just out of reach, and you’re standing there saying, “You know, the thing, the…” while your colleagues wait patiently. You feel incompetent and embarrassed.
You make a grocery list because you know you’ll forget otherwise. Then you forget the list at home. At the store, you wander the aisles trying to remember what you needed, buying random things that seem familiar, only to get home and realize you forgot the main ingredient for dinner.
You’re watching a show you love and realize you have no idea what just happened in the last ten minutes. You were staring at the screen, but your mind was completely blank. You rewind and still can’t concentrate enough to follow the plot.
Women describe brain fog as feeling like something’s clouding their ability to think clearly, affecting memory, focus, and overall mental clarity. It’s not one dramatic symptom; it’s a collection of small cognitive frustrations that add up to feeling like you’re not yourself anymore.
The scariest part? Many of us immediately jump to thinking this is early dementia. Some women become so concerned that they’re referred to memory clinics for testing, and the fear itself becomes another layer of stress that makes the brain fog worse.
Why your brain is acting this way
Here’s what’s actually happening in your brain during perimenopause, explained in a way that makes sense without a medical degree.
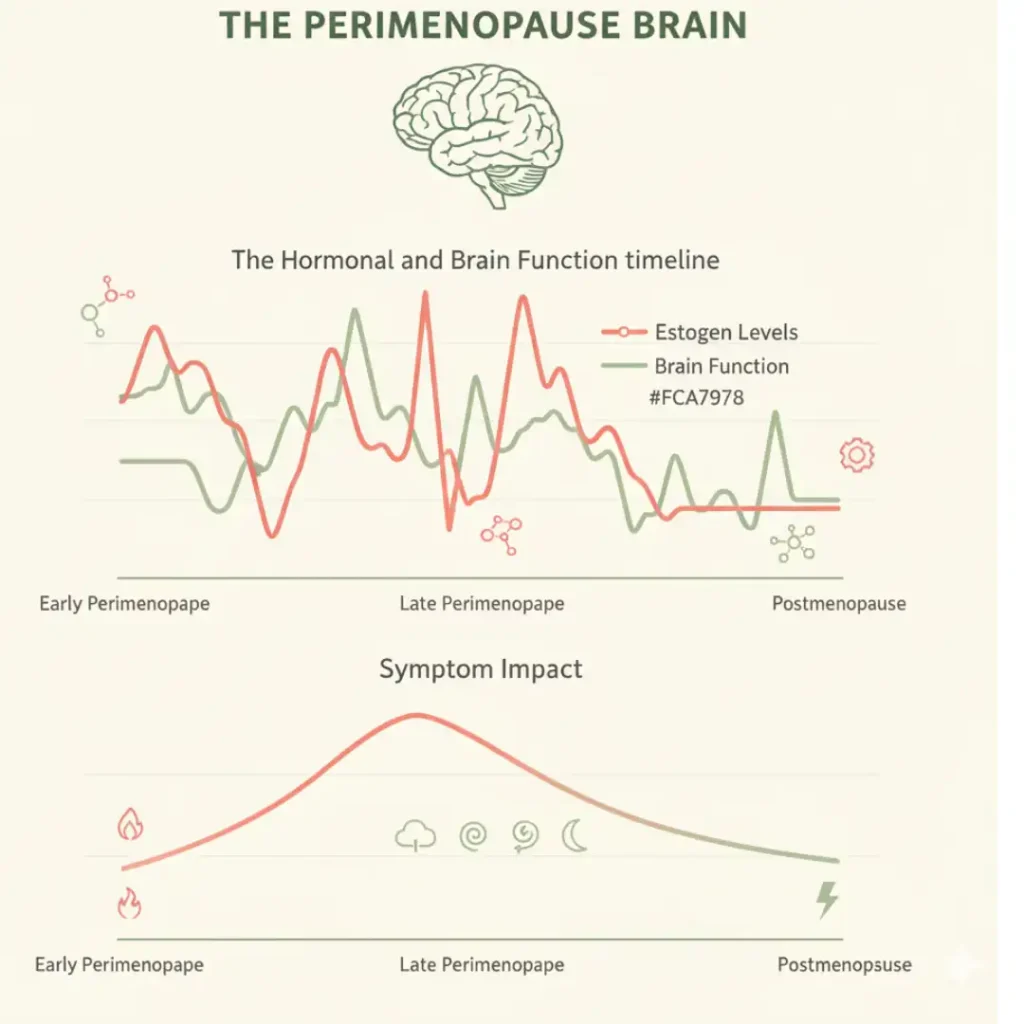
Estrogen and testosterone play important roles in cognition and memory. When their levels begin to fall during perimenopause, this leads to various cognitive symptoms, including memory loss, difficulty staying focused, and word-finding difficulties.
Think of estrogen as fuel for your brain. It stimulates the brain, keeps neurons firing, supports the growth of new cells, and helps existing cells form new connections. During perimenopause, your estrogen levels don’t just drop steadily; they fluctuate wildly. Some days you have plenty, other days you’re running on empty. Your brain is constantly trying to adjust to these unpredictable changes.
Here’s the part that really helped me understand what I was experiencing: estrogen pushes your brain cells to burn more glucose, which is the brain’s main fuel. When estrogen drops, there’s an overall reduction in brain energy levels. It’s like trying to run your computer on a low battery; everything slows down and doesn’t work as smoothly.
The testosterone connection surprised me. I always thought of testosterone as a male hormone, but women produce it too, and it matters for brain function. Testosterone strengthens nerves in the brain and contributes to mental sharpness and clarity. When it declines along with estrogen, that’s another hit to your cognitive function.
Research shows that verbal learning and verbal memory are the cognitive functions most negatively affected during perimenopause. That’s why you might find yourself struggling to remember names, losing words mid-sentence, or having trouble retaining information you just read.
The good news that helped me stop panicking: this brain fog probably won’t last, and studies suggest perimenopausal women temporarily have trouble learning new information, but it gets better with time as women get past menopause.
The sleep connection you can’t ignore
Let’s talk about something that makes perimenopause brain fog dramatically worse: terrible sleep.
I went through a phase where I’d wake up at 3 AM every single night, wide awake for two hours, then finally fall back asleep twenty minutes before my alarm went off. I’d drag myself through days feeling like I was underwater, my thinking even foggier than usual. If you’re experiencing similar sleep struggles, you’re not alone, and understanding Why Can’t I Sleep Anymore can help you find solutions that work.
It’s common to have trouble sleeping during perimenopause because the brain can’t regulate sleep properly without estrogen and progesterone. If you’re struggling to fall asleep, waking up repeatedly, or experiencing those frustrating middle-of-the-night wake-ups, you’re missing out on deep sleep that’s essential for brain health.
Here’s why this matters so much: deep sleep is when all the toxins and impurities are removed from the brain. This phase of sleep is essential for keeping the brain healthy. Without enough deep sleep, your brain can’t perform its nightly cleanup and maintenance. No wonder everything feels cloudy the next day.
Brain fog can be linked to sleep disturbances, and many women notice that once their sleep improves, their cognitive complaints improve too.
I noticed this pattern in my own experience. On rare nights when I slept well, my thinking was noticeably clearer the next day, I could focus better, remember things more easily, and didn’t struggle as much to find words. The brain fog wasn’t completely gone, but it was significantly lighter.
Improving sleep became one of my top priorities, not just because I was exhausted, but because I realized how directly it affected my cognitive function; small changes made a real difference. I started keeping my bedroom cooler, limiting screen time before bed, and creating a more consistent sleep routine. None of these things fixed the problem entirely, but together they helped me get more restorative sleep more often.
What actually helps with brain fog
I’m going to be honest with you. No magic pill makes perimenopause brain fog disappear overnight. What works is a combination of strategies that support your brain during this transition.
Let me share what made a real difference for me and what research shows actually helps.
Start with omega-3 fatty acids. Research has found that regular omega-3 consumption is associated with better cognitive performance and reduced inflammation in menopausal women. I added salmon to my diet twice a week and started taking a quality fish oil supplement after talking to my doctor. Within a few weeks, I noticed my thinking felt slightly sharper. Not dramatically different, but noticeably better.
If fish isn’t your thing, you can get omega-3s from plant sources like flaxseeds, chia seeds, and walnuts. I sprinkle ground flaxseed on my yogurt every morning; it’s a small habit that supports brain health without requiring much effort.
Movement matters more than I expected. Regular exercise increases blood flow to the brain, stimulates the growth of new brain cells, and releases mood-enhancing chemicals that can help clear mental fog. I’m not talking about intense workouts that feel like punishment. I started walking for 30 minutes most mornings, and on days when I moved my body, my brain worked better.
The connection between physical activity and mental clarity is real. On days when I skipped my walk, I noticed the brain fog felt heavier. Exercise doesn’t have to be complicated. Walking, swimming, gentle yoga, whatever gets your body moving and your blood flowing.
Here’s something that surprised me: mindfulness meditation improved working memory and reduced mental fatigue in menopausal women. I was skeptical at first because meditation felt like one more thing I was supposed to do perfectly. But I started with just five minutes a day, focusing on my breath, and it genuinely helped me feel more mentally present.
Stress management became non-negotiable; panicking about thinking and memory issues can actually make them worse. When I stopped catastrophizing every time I forgot something and started responding with “oh, this is just perimenopause,” my anxiety decreased, and my cognitive function actually improved slightly.
Challenge your brain regularly. Taking different routes to familiar destinations and changing up your routine helps create new memories and new processes rather than always going by habit. I started taking different streets to the grocery store, trying new recipes, and doing crossword puzzles. Keeping my brain engaged and creating new neural pathways seemed to help maintain cognitive function.

Foods that support your brain
What you eat directly affects how your brain functions during perimenopause. I’m not talking about a restrictive diet; I’m talking about adding foods that give your brain what it needs.
Oily fish rich in omega-3 essential fatty acids and folate are vital for brain and nervous system functioning, including sardines, salmon, herring, anchovies, and mackerel. I know not everyone loves fish, but if you can incorporate it a couple of times a week, your brain will thank you.
Here’s something interesting: eating soy has been shown to improve memory in menopausal women. I started adding edamame as a snack and using tofu in stir-fries more often. These small dietary additions felt manageable rather than overwhelming.
Cut back on processed foods and added sugars. I noticed that on days when I ate a lot of sugary snacks or processed foods, my brain fog felt worse. When I focused on whole foods, vegetables, lean proteins, and healthy fats, my mental clarity improved. It wasn’t dramatic, but it was noticeable. Understanding Weight Loss After Menopause can make a significant difference in how you feel mentally and physically.
Think of food as information you’re giving your brain; quality information leads to better function. You don’t have to be perfect, but making more brain-supporting food choices more often really does make a difference.
When to worry and when to relax
Let me address the fear that’s probably lurking in the back of your mind: how do you know this is perimenopause brain fog and not something more serious?
Brain fog appears to be temporary, and tests for brain fog after the menopause transition show improvement. This is crucial information. For most women, these cognitive symptoms improve once hormones stabilize after menopause.
Here’s what’s normal perimenopause brain fog: forgetting where you put your keys, losing words occasionally, having trouble concentrating when reading, needing to make lists for everything, and feeling mentally fuzzy at times.
Here’s what warrants a conversation with your doctor: forgetting how to do routine tasks you’ve done for years, getting lost in familiar places, significant personality changes, forgetting the names of close family members, and struggling with basic daily activities.
I went to my doctor when my brain fog was at its worst, terrified something was seriously wrong. She did a full evaluation and confirmed that what I was experiencing was consistent with perimenopause; that reassurance alone reduced my anxiety significantly, which in turn reduced the intensity of my symptoms.
More than 60 percent of women experience brain fog at some point during perimenopause or menopause. You’re not alone in this experience, and for the vast majority of women, it’s a temporary phase that resolves.
If your brain fog is significantly impacting your work performance or daily life, talk to your doctor about treatment options. Hormonal therapy may help ease symptoms, and many women notice improvement in their cognitive complaints once other menopausal symptoms like hot flashes and sleep issues are better controlled.
Building your personal strategy
What works for brain fog varies widely. What helped me might not be exactly what helps you, but the principles are the same: support your brain during this transition.
Start by improving your sleep; this may involve consulting your doctor about sleep issues, establishing a more consistent bedtime routine, or addressing nighttime sweats that disrupt your sleep. Quality sleep is foundational for cognitive function.
Add omega-3s through food or supplements. This is backed by solid research and has made a noticeable difference for me.
Move your body regularly in ways you actually enjoy. The best exercise is the one you’ll actually do consistently.
Manage stress through whatever works for you: meditation, yoga, walks in nature, time with friends, therapy. Chronic stress makes everything worse, including brain fog. Developing a resilient mindset during this transition helps you respond to symptoms with self-compassion rather than panic.
Challenge your brain with new activities and learning. Keep those neural pathways active and forming new connections.
Be patient and compassionate with yourself. Awareness is valuable, but be gentle with yourself, as Menopause after 50 is a significant life transition, and midlife changes in the brain and body are a natural part of the process.
Write things down without shame. I started keeping a small notebook with me everywhere. There’s no prize for remembering everything in your head during perimenopause. External memory aids are tools, not failures.
Connect with other women going through this. When I started talking openly about my brain fog, I discovered so many friends were experiencing the same thing. Knowing I wasn’t alone helped enormously.
Most importantly, understand this is temporary. Your brain is adapting to significant hormonal changes, and once it adjusts, your cognitive function will improve. You’re not broken, you’re transitioning.
For a deeper understanding of how hormonal changes like perimenopause connect to your overall mental well-being and what you can do to support yourself through this transition, I encourage you to explore more about the mind-body connection during this life stage.
Frequently asked questions
You’re not losing your mind, you’re adapting
I want to close by returning to that moment in the Target parking lot when I couldn’t find my car and sat crying behind the wheel.
That moment felt like rock bottom. I genuinely thought something was seriously wrong with me. But looking back now, I see it differently. That was the moment I stopped dismissing my symptoms and started taking them seriously. It was the moment I began learning about what was actually happening in my body and brain.
Perimenopause brain fog is real, it’s common, and it’s temporary. Understanding the biological reality of what’s happening, that your brain is adapting to significant hormonal changes, takes away some of the fear. You’re not failing, you’re transitioning.
The strategies that help aren’t complicated or expensive: better sleep, omega-3s, regular movement, stress management, brain challenges, and self-compassion. None of these things will transform your brain fog overnight, but together, consistently, they make a real difference.
Your brain is remarkably adaptable. It will adjust to these hormonal changes. The fog will lift. In the meantime, be gentle with yourself, use whatever tools and strategies help you function better, and remember that you’re navigating one of life’s major transitions.
If you’re struggling significantly, please talk to your doctor. There are treatment options that can help, and you deserve support during this challenging phase. Professional help isn’t a sign of weakness; it’s a sign of wisdom.
For a deeper understanding of how your mindset shapes your experience of this life stage, including how you cope with symptoms like brain fog, explore our comprehensive guide thriving after 50.
What’s one strategy you’re going to try this week to support your brain? I’d love to hear what’s working for you.



